|
But when she called, a Cigna representative told her the hospital had changed the billing code for her procedure from screening to diagnostic. She hadn't owed anything after her first colonoscopy. Resolution: When Melville received notices about owing $2,185, she initially thought it must be a mistake. The key difference between the two experiences: Melville's husband didn't have a polyp removed. Despite his family history of colon cancer and a previous colonoscopy just five years earlier because of his elevated risk, her husband wasn't charged anything for the test. In addition, getting a screening colonoscopy sooner than the recommended 10-year interval, as Melville did, could open someone up to cost-sharing charges, Howard said.Ĭoincidentally, Melville's 61-year-old husband had a screening colonoscopy at the same facility with the same doctor a week after she had her procedure. "Right from the start, could be considered diagnostic," Howard said. Having a family history of colon cancer or a personal history of polyps raises someone's risk profile, and insurers and providers could impose charges based on that. Someone whose cancer risk is above average may face higher bills and not be protected by the law, said Anna Howard, a policy principal at the American Cancer Society's Cancer Action Network. More than 40% of people over 50 have precancerous polyps in the colon, according to the American Society for Gastrointestinal Endoscopy. Here's How To Do ItĪfter all, that's the whole point of screening - to figure out whether polyps contain cancer, they must be removed and examined by a pathologist. Life Kit Getting Out Of Medical Debt Can Feel Impossible. 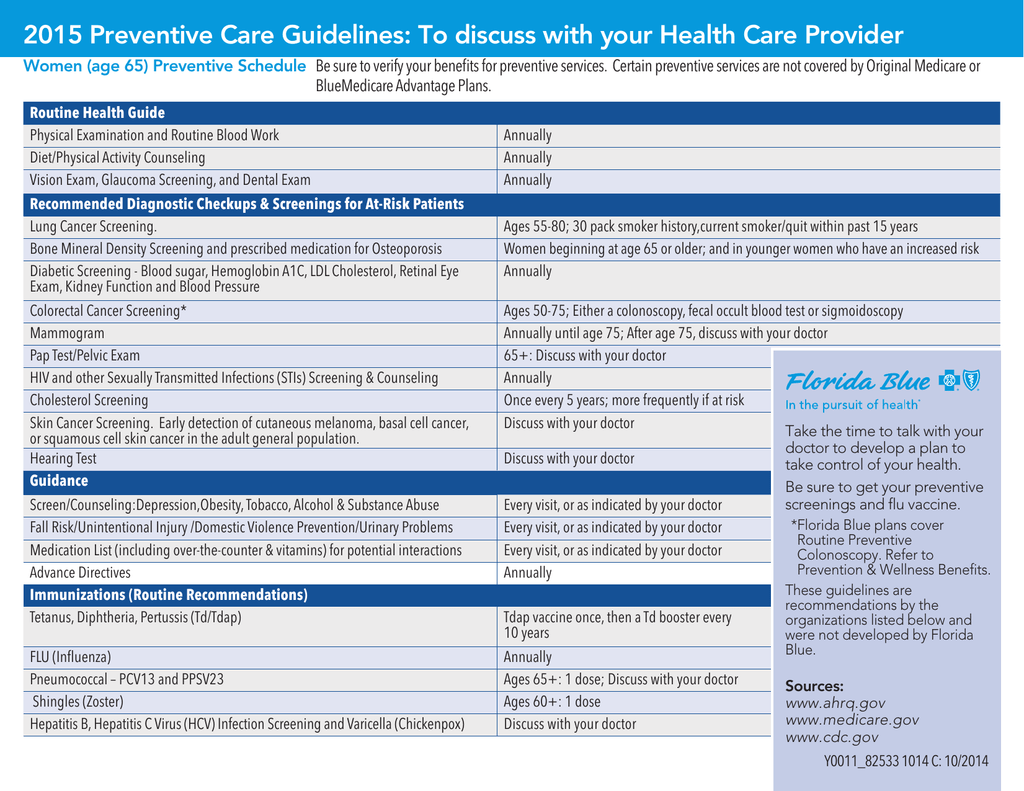
The Centers for Medicare & Medicaid Services has clarified repeatedly over the years that under the preventive services provisions of the ACA, removal of a polyp during a screening colonoscopy is considered an integral part of the procedure and should not change patients' cost-sharing obligations. The former generally incurs no cost to patients under the ACA the latter can generate bills. How they are classified makes all the difference for patients' out-of-pocket costs. Preventive Services Task Force, a nonpartisan group of medical experts, recommends regular colorectal cancer screening for average-risk people from ages 45 to 75.Ĭolonoscopies can be classified as for screening or for diagnosis. Screening colonoscopies reduce the relative risk of getting colorectal cancer by 52% and the risk of dying from it by 62%, according to a recent analysis of published studies. Getting screened regularly for colorectal cancer is one of the most effective tools people have for preventing it. Often the doctors and hospitals are the ones who decide when those categories shift and a patient can be charged - but those decisions often are debatable. 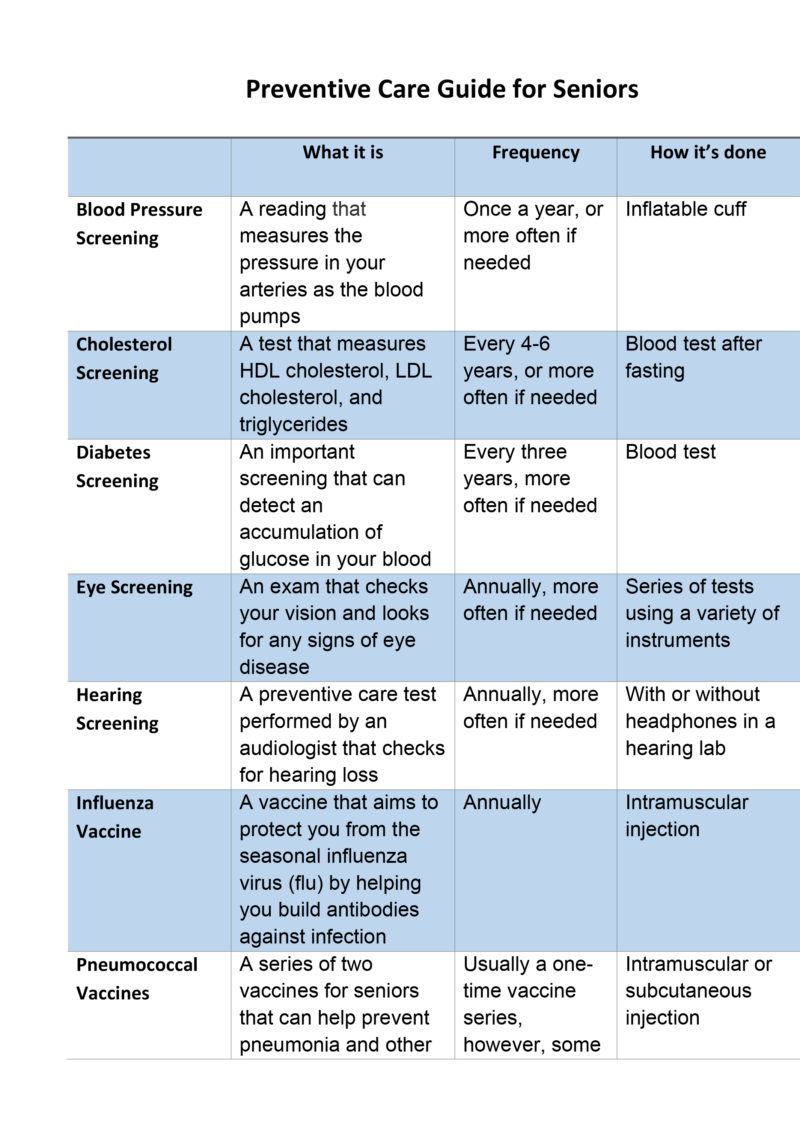
But there is wiggle room to charge when a procedure is done for diagnosis versus for screening purposes. What Gives: The Affordable Care Act made preventive health care such as mammograms and colonoscopies free of charge to patients without cost sharing. Cigna's negotiated rate was $4,144, and Melville's share under her insurance was $2,185. Total Bill: $10,329 for the procedure, anesthesiologist, and gastroenterologist. It is part of the Dartmouth Health system, a nonprofit academic medical center and regional network of five hospitals and more than 24 clinics with nearly $3 billion in annual revenue. Service Provider: New London Hospital, a 25-bed facility in New London, New Hampshire. Medical Service: A screening colonoscopy, including removal of a benign polyp. It has a $2,500 individual deductible and 30% coinsurance. The Patient: Elizabeth Melville, 59, is covered under a Cigna health plan that her husband gets through his employer.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
